|
January 2021
Changes coming Jan. 1 for preferred, clinical, custom and custom select drug lists
We recently published an article that detailed changes to the Preferred Drug List, starting Jan. 1, 2021. We’re making an update to the exclusion information: Cimzia® and Kevzara® will remain on the Preferred Drug List. These drugs won’t be excluded.
Preferred Drug List changes
The following tables show the Preferred Drug List changes that are effective Jan. 1, 2021.
Drugs no longer covered – Preferred Drug List
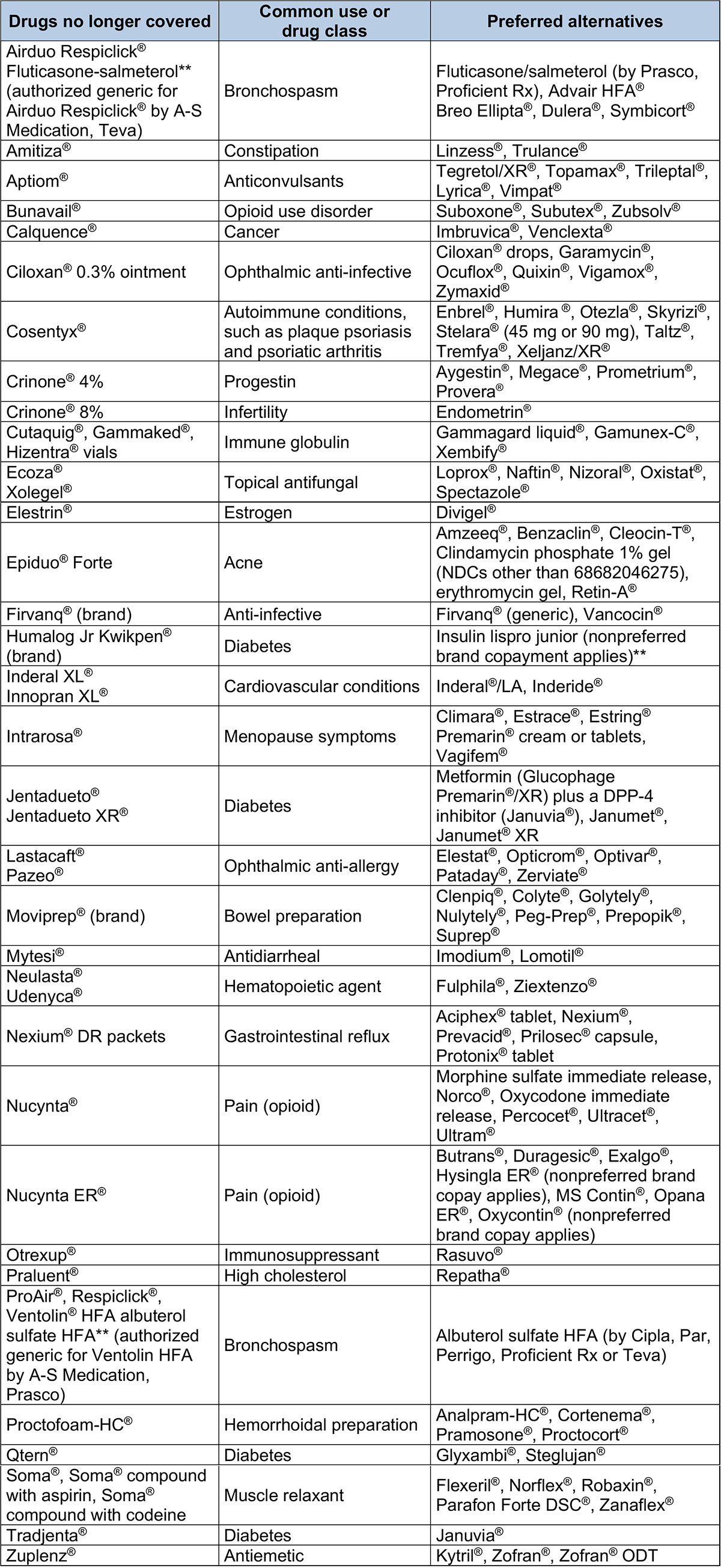
We’ll no longer cover the following brand-name and generic drugs. If a member fills a prescription for one of these drugs on or after Jan. 1, 2021, he or she will be responsible for the full cost. The list below shows preferred alternatives that have similar effectiveness, quality and safety. Unless noted, we won’t cover both the brand-name and available generic equivalents. The example brand names of preferred alternatives are for your reference. When a prescription is filled, the generic equivalent is dispensed, if available.
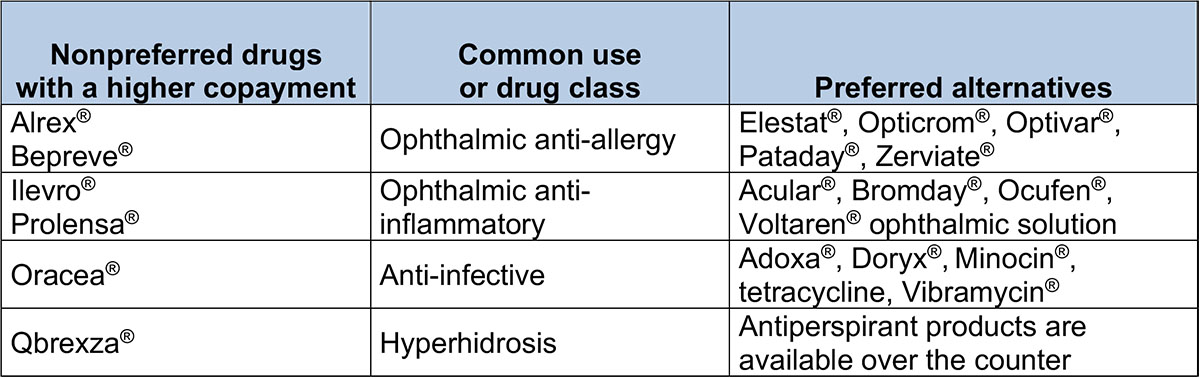
Drugs with a higher copayment – Preferred Drug List
The brand-name drugs with a higher copayment are listed below along with the preferred alternatives with similar effectiveness, quality and safety. The example brand names of preferred alternatives are for your reference. When a prescription is filled, the generic equivalent is dispensed, if available.
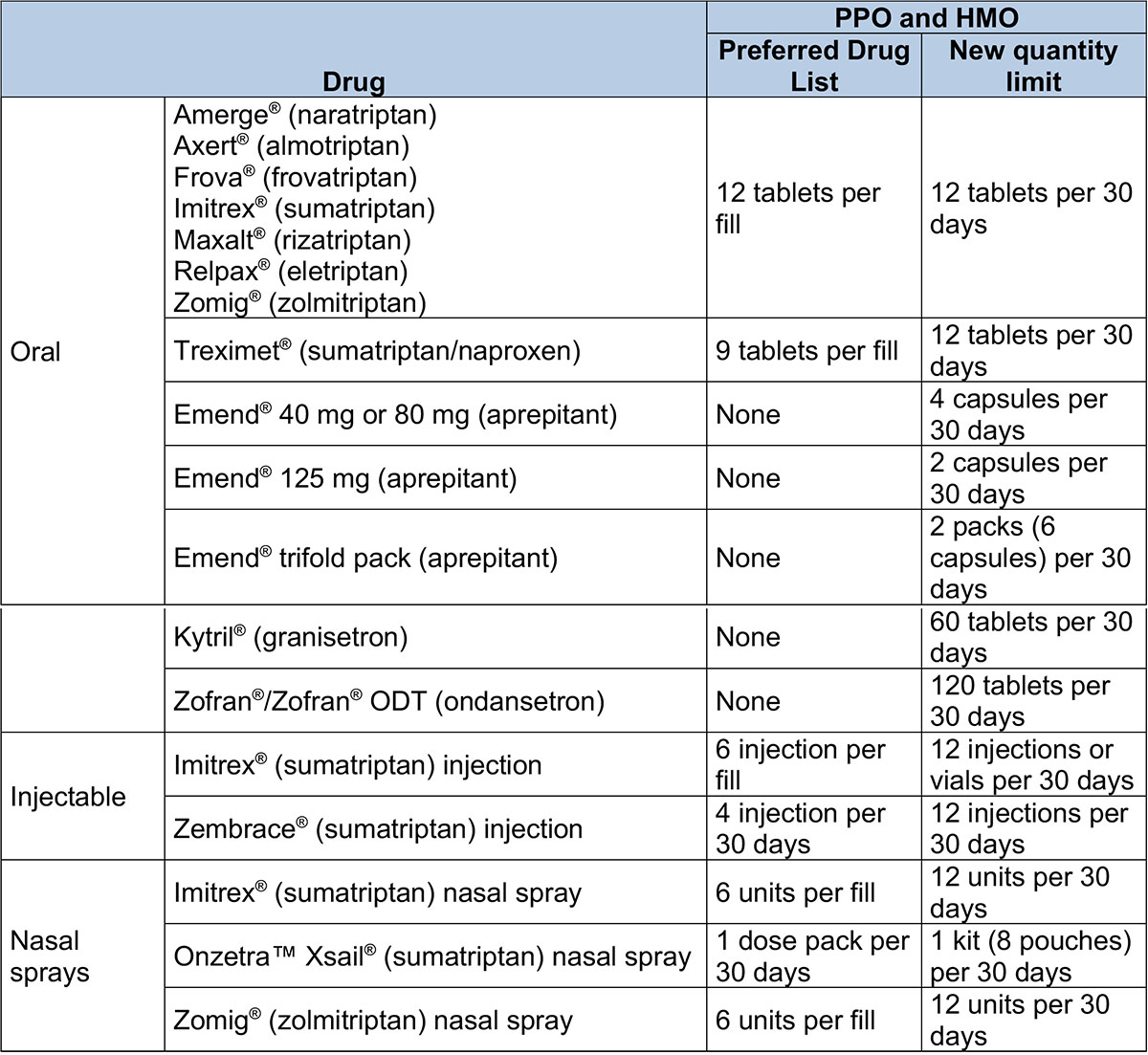
Drugs with quantity limits – Preferred Drug List
These drugs have changes to the amount that can be filled.
Clinical, Custom and Custom Select Drug List changes
The following tables show the changes that are effective starting Jan. 1, 2021, for the Clinical, Custom or Custom Select Drug lists.
Drugs no longer covered – Clinical and Custom Drug lists
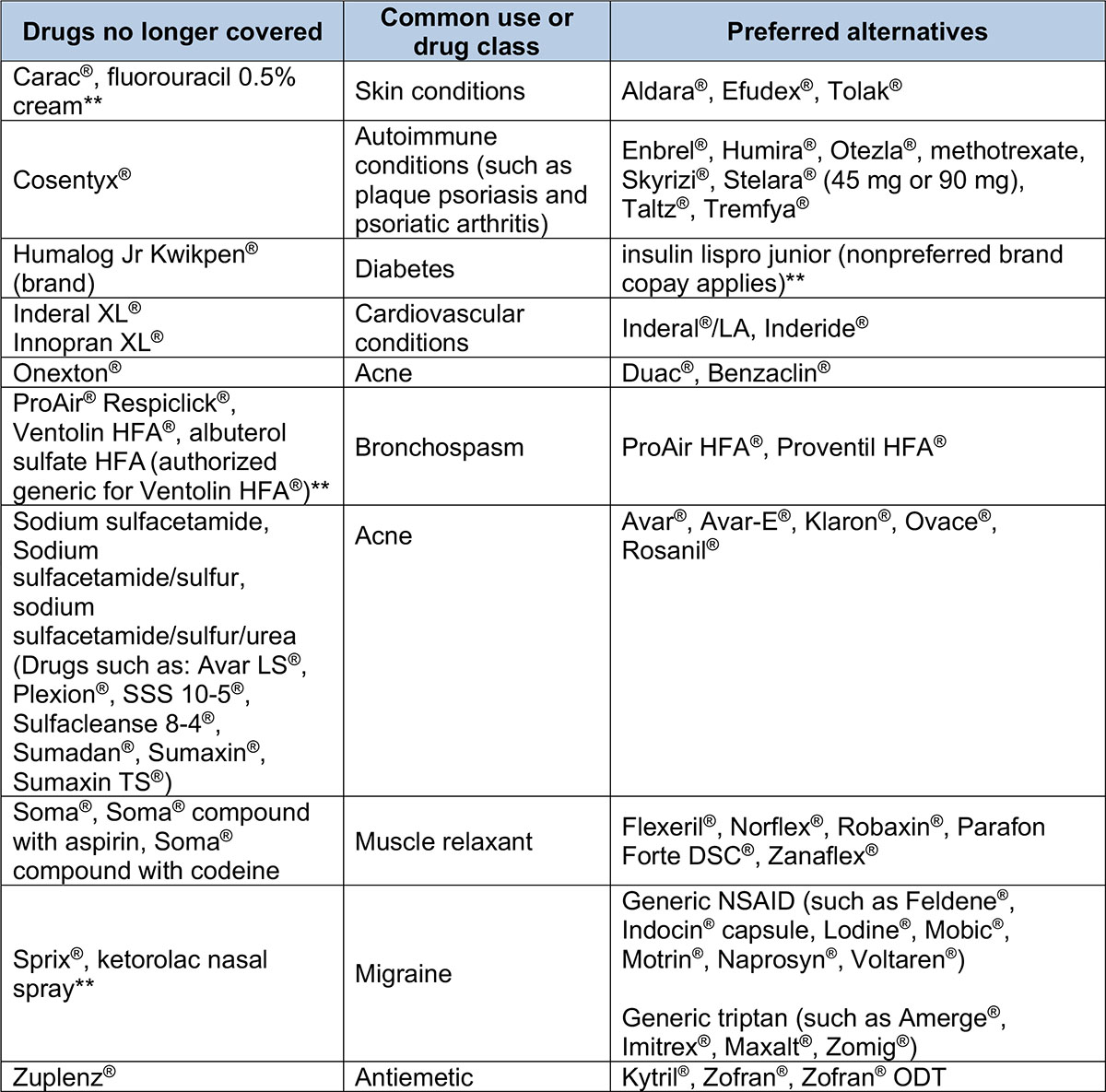
We’ll no longer cover the following brand-name and generic drugs. If a member fills a prescription for one of these drugs on or after Jan. 1, 2021, he or she will be responsible for the full cost. The list shows preferred alternatives that have similar effectiveness, quality and safety. Unless noted, we won’t cover both the brand-name and available generic equivalents. The example brand names of preferred alternatives are for your reference. When a prescription is filled, the generic equivalent is dispensed, if available.
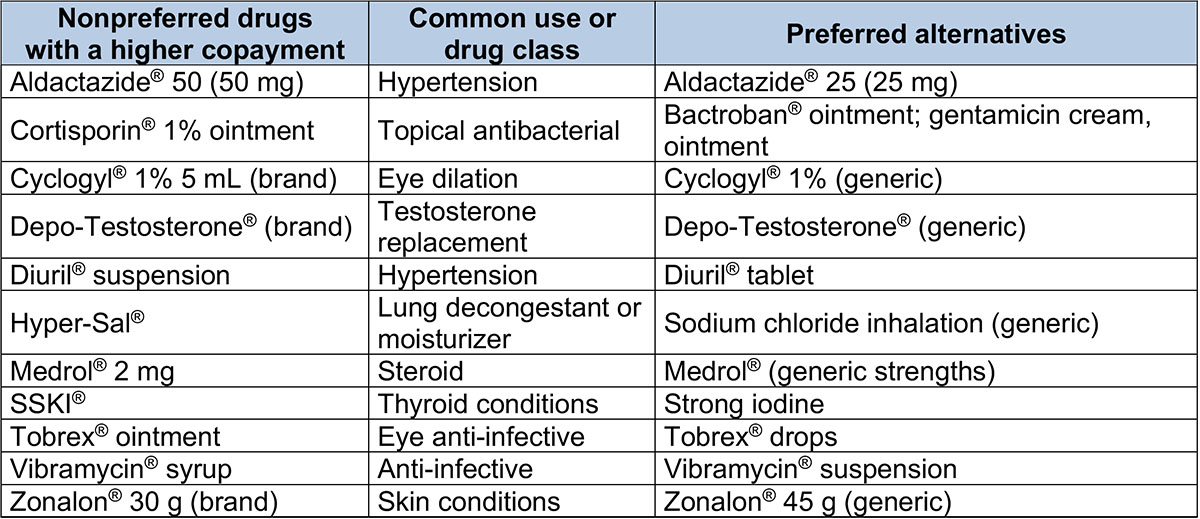
Drugs with a higher copayment – Custom Drug List
The brand-name drugs with a higher copayment are listed below along with the preferred alternatives that have similar effectiveness, quality and safety. The example brand names of preferred alternatives are for your reference. When a prescription is filled, the generic equivalent is dispensed, if available.
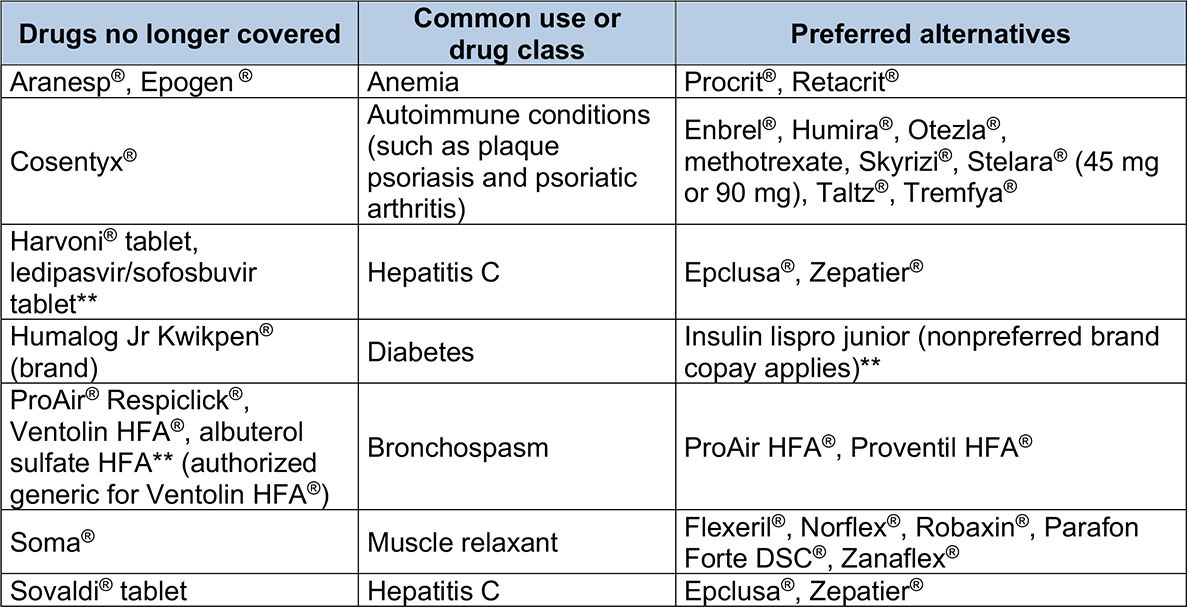
Drugs no longer covered – Custom Select Drug List
We’ll no longer cover the following brand-name and generic drugs. If a member fills a prescription for one of these drugs on or after Jan. 1, 2021, he or she will be responsible for the full cost. The list shows preferred alternatives with similar effectiveness, quality and safety. Unless noted, we won’t cover both the brand-name and available generic equivalents. The example brand names of preferred alternatives are for your reference. When a prescription is filled, the generic equivalent is dispensed, if available.
Drugs with quantity limits – Clinical, Custom and Custom Select Drug lists
These drugs have changes to the amount that can be filled:
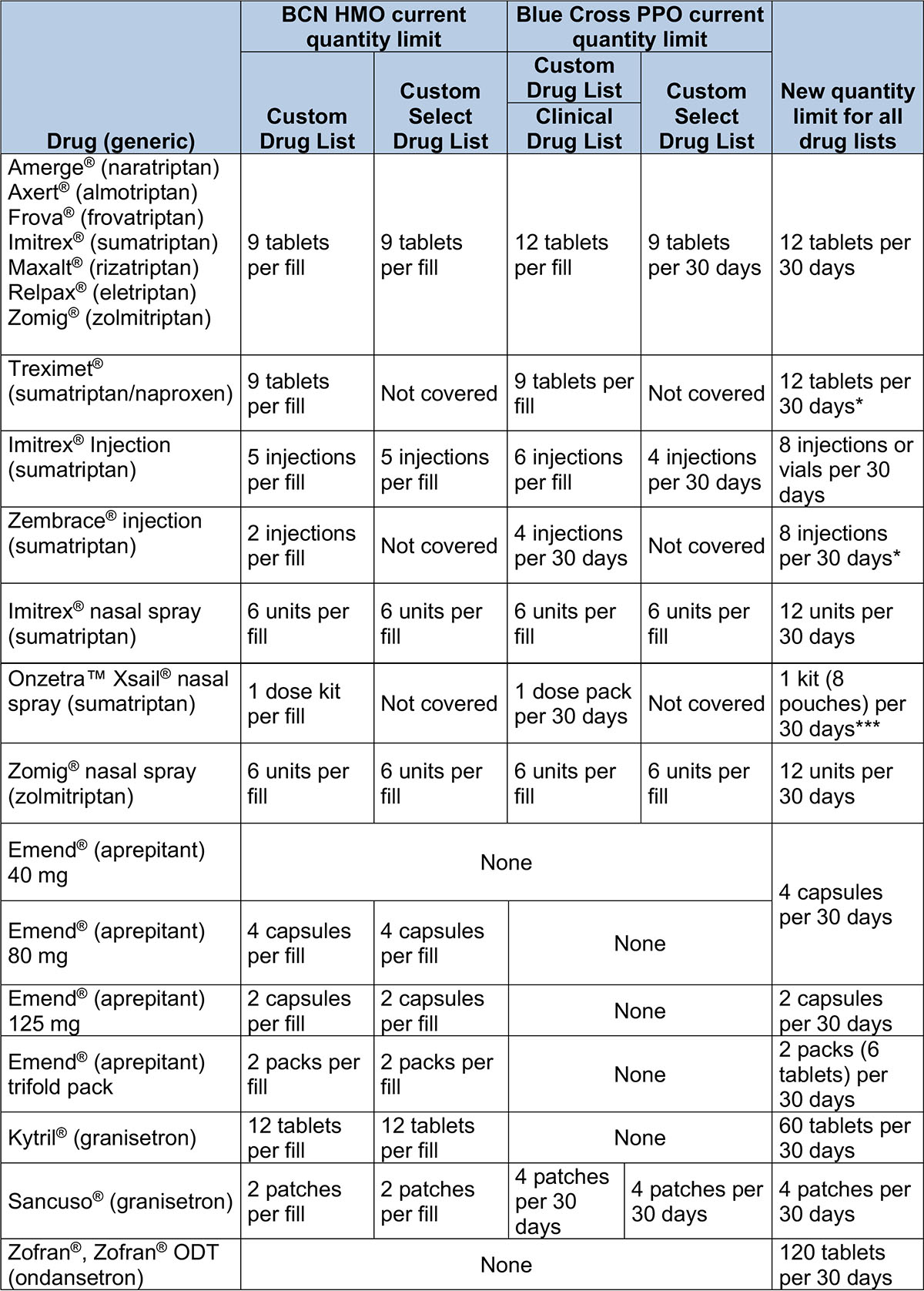
**Represents drugs that have brand names without generic equivalents. These may be considered “authorized generics,” which are the same as brand-name drugs but aren’t true generic drugs.
***Doesn’t apply to members whose plans use the Custom Select Drug List.
|







