|
November 2020
Starting Jan. 1, 2021, we’re changing how we cover some drugs
The health of our members is important to Blue Cross Blue Shield of Michigan and Blue Care Network. We want to ensure safe, high-quality care to meet their needs. As part of our efforts, we’re making some changes to how we cover certain drugs on the Clinical, Custom, Custom Select and Preferred Drug Lists, starting Jan. 1, 2021. We’ll send letters to affected members and health care providers about these changes.
Here’s an overview:
Drugs on the Preferred Drug List that won’t be covered
We’ll no longer cover the following brand-name and generic drugs. If a member fills a prescription for one of these drugs on or after Jan. 1, 2021, he or she will be responsible for the full cost. The drugs that won’t be covered are listed. Unless noted, both the brand-name and available generic equivalent drugs won’t be covered. Also listed are preferred alternatives with similar effectiveness, quality and safety. The examples brand names of preferred alternatives are provided for reference. When a prescription is filled, the generic equivalent is dispensed, if available.
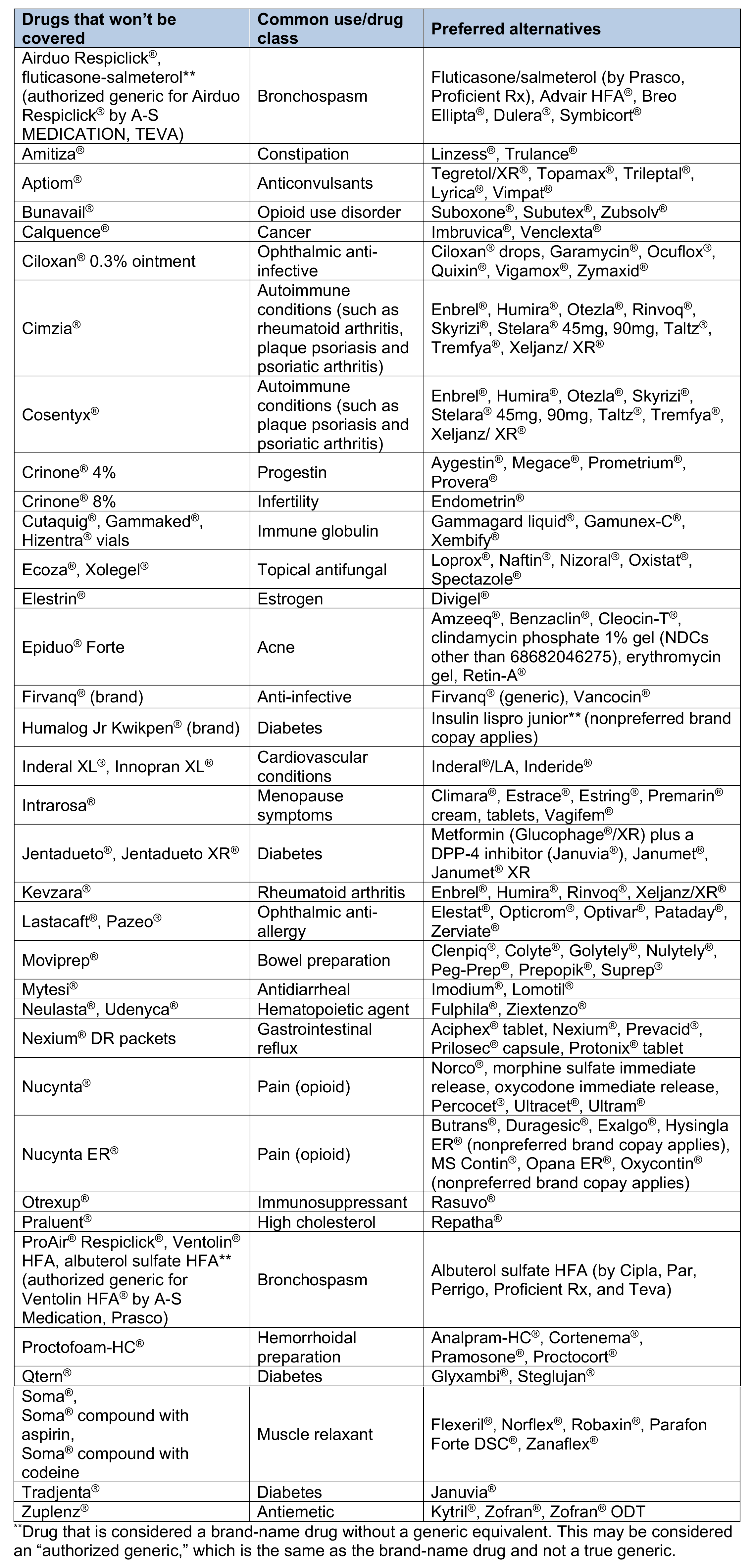
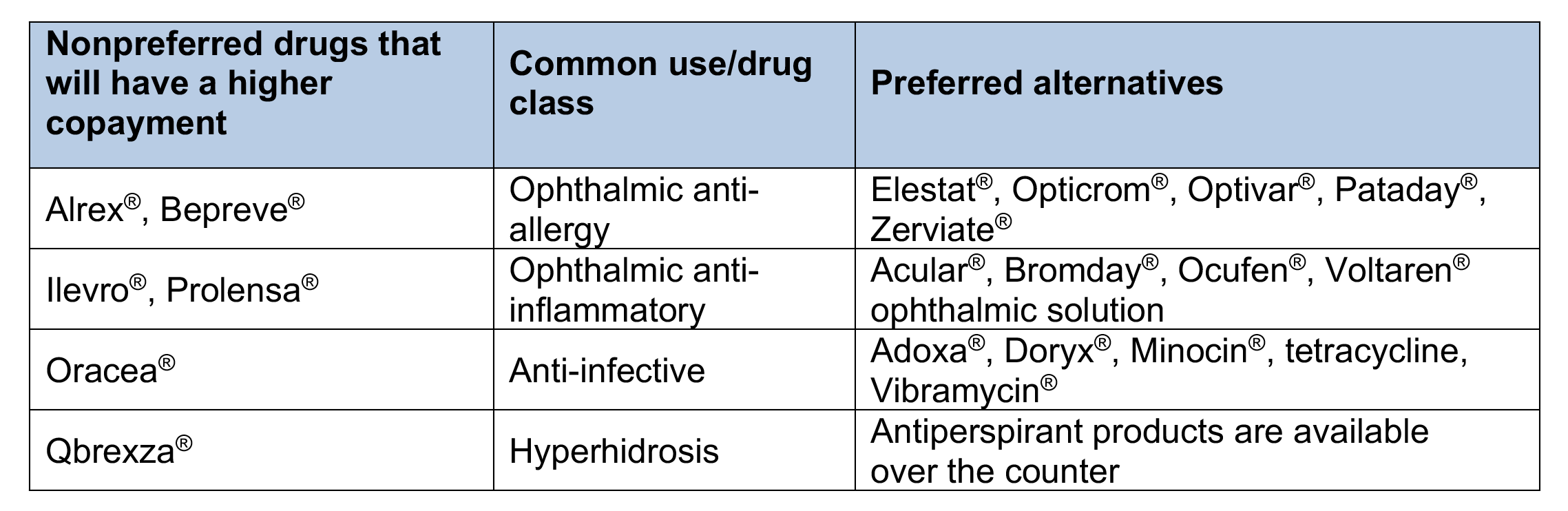
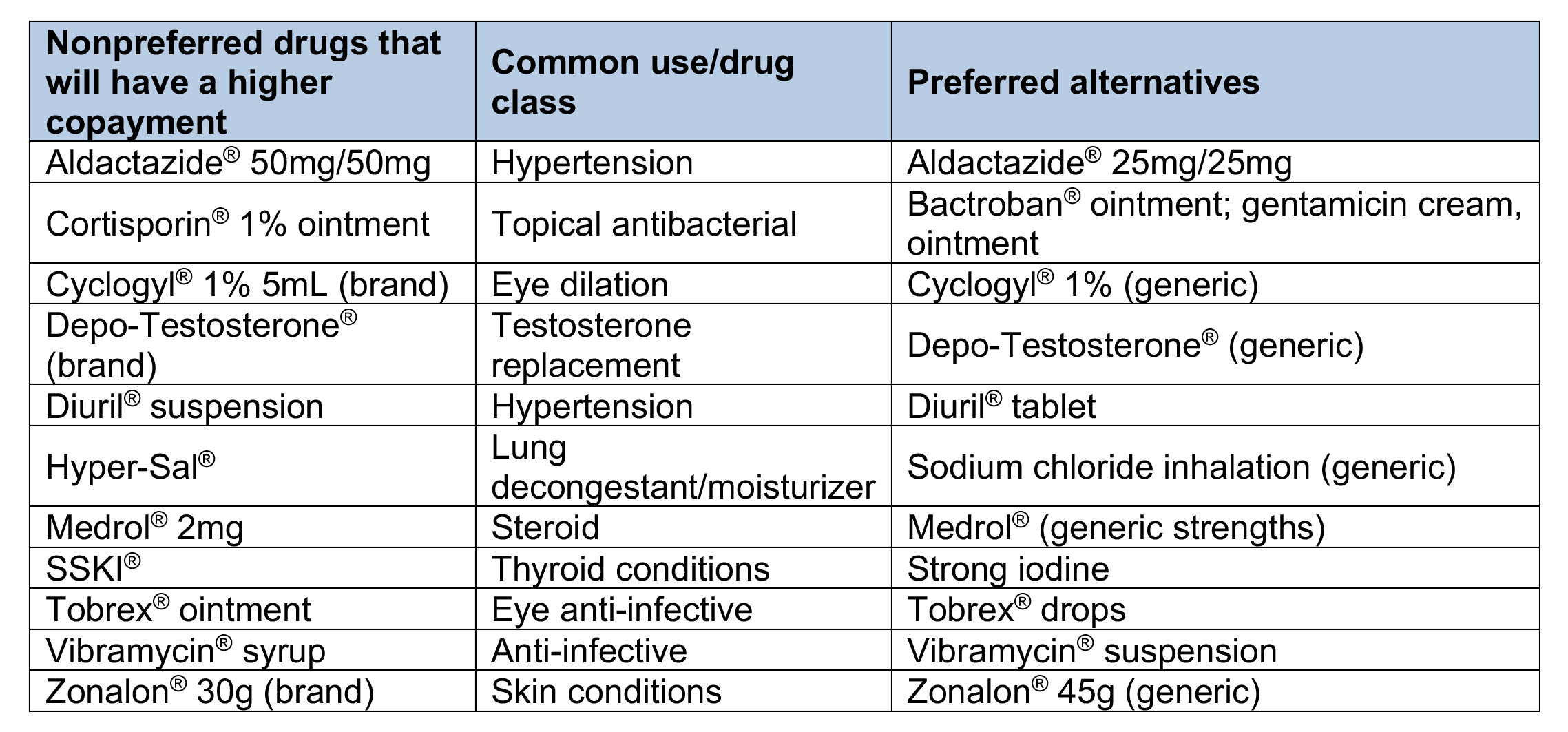
Drugs on the Preferred Drug List that will have a higher copayment
The brand-name drugs that have a higher copayment are listed, along with the preferred alternatives that have similar effectiveness, quality and safety. The example brand names of preferred alternatives are provided for reference. When a prescription is filled, the generic equivalent is dispensed, if available.
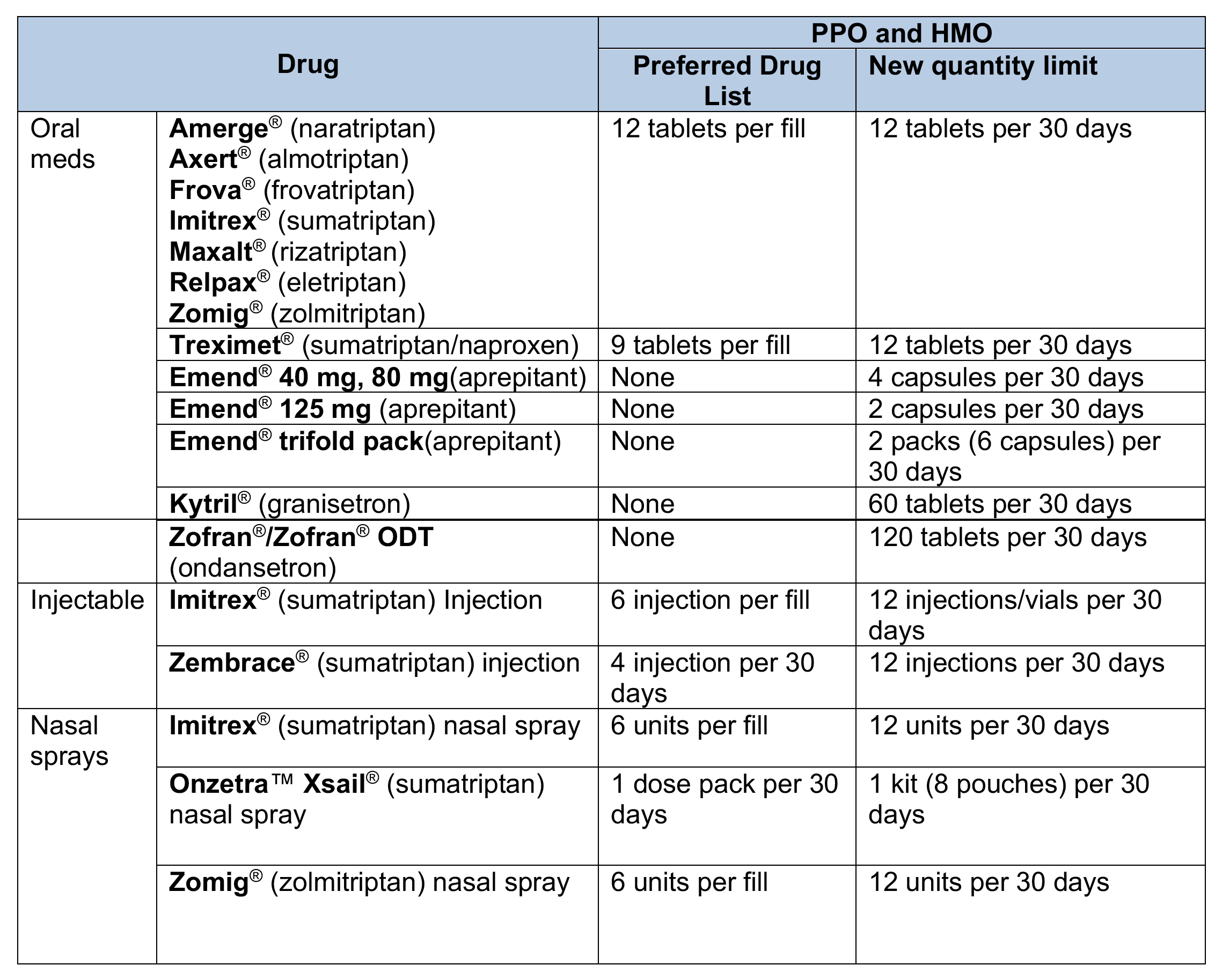
Drugs on the Preferred Drug List that will have quantity limits
These drugs will have changes to the amount that can be filled.
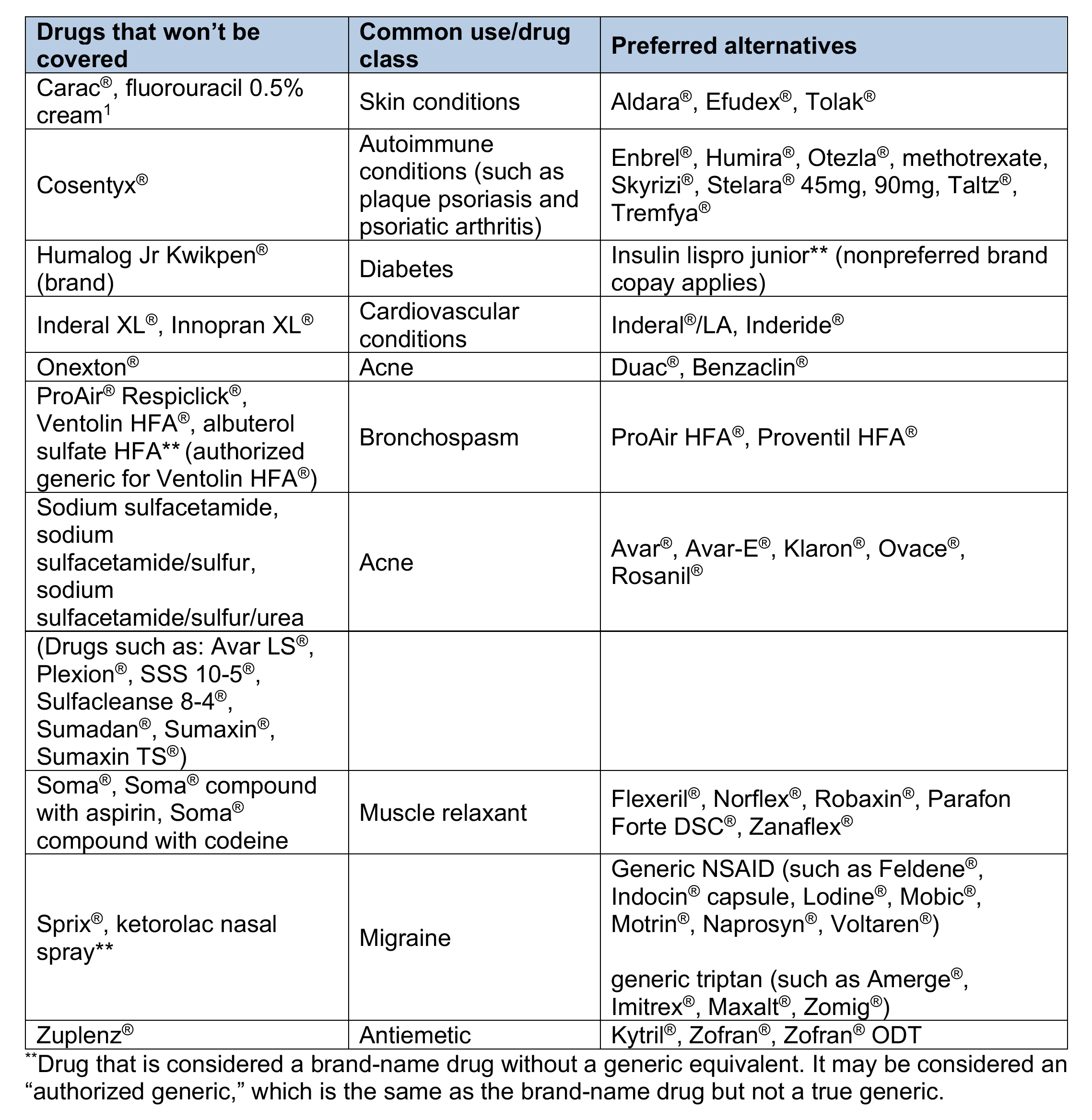
Drugs on the Clinical and Custom Drug Lists that won’t be covered
We’ll no longer cover the following brand-name and generic drugs. If a member fills a prescription for one of these drugs on or after Jan. 1, 2021, he or she will be responsible for the full cost. The drugs that won’t be covered are listed and, unless noted, both the brand-name and available generic equivalent drugs won’t be covered. The preferred alternatives that have similar effectiveness, quality and safety are also listed. The example brand names of preferred alternatives are provided for reference. When a prescription is filled, the generic equivalent is dispensed, if available.
Drugs on the Custom Drug List that will have a higher copayment
The brand-name drugs that will have a higher copayment are listed, along with the preferred alternatives that have similar effectiveness, quality and safety. The example brand names of preferred alternatives are provided for reference. When a prescription is filled, the generic equivalent is dispensed, if available.
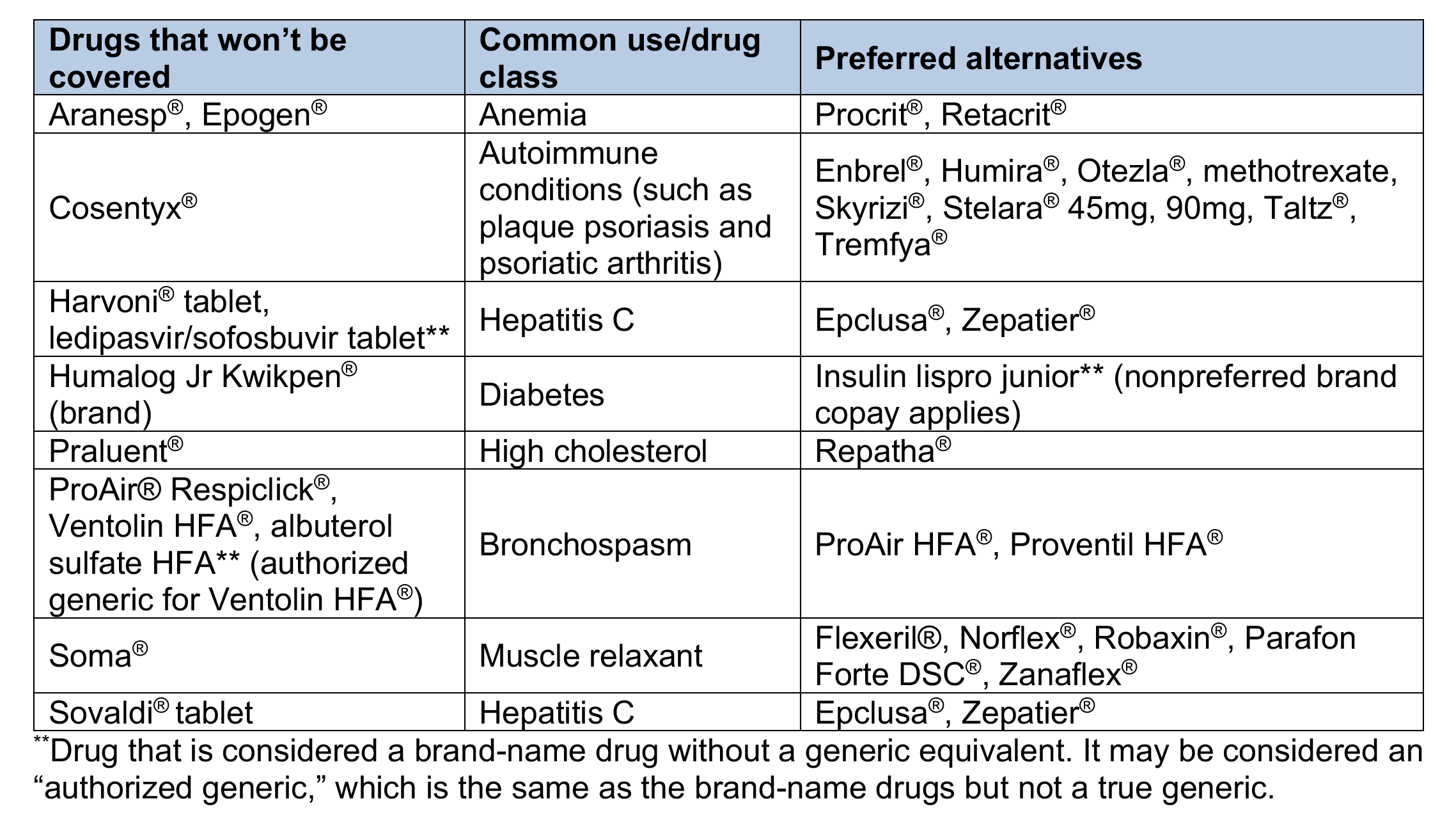
Drugs on the Custom Select Drug List that won’t be covered
We’ll no longer cover the following brand-name and generic drugs. If a member fills a prescription for one of these drugs on or after Jan. 1, 2021, he or she will be responsible for the full cost. The drugs that won’t be covered are listed and, unless noted, both the brand-name and available generic equivalent drugs won’t be covered. Preferred alternatives that have similar effectiveness, quality and safety are listed. The example brand names of preferred alternatives are provided for reference. When a prescription is filled, the generic equivalent is dispensed, if available.
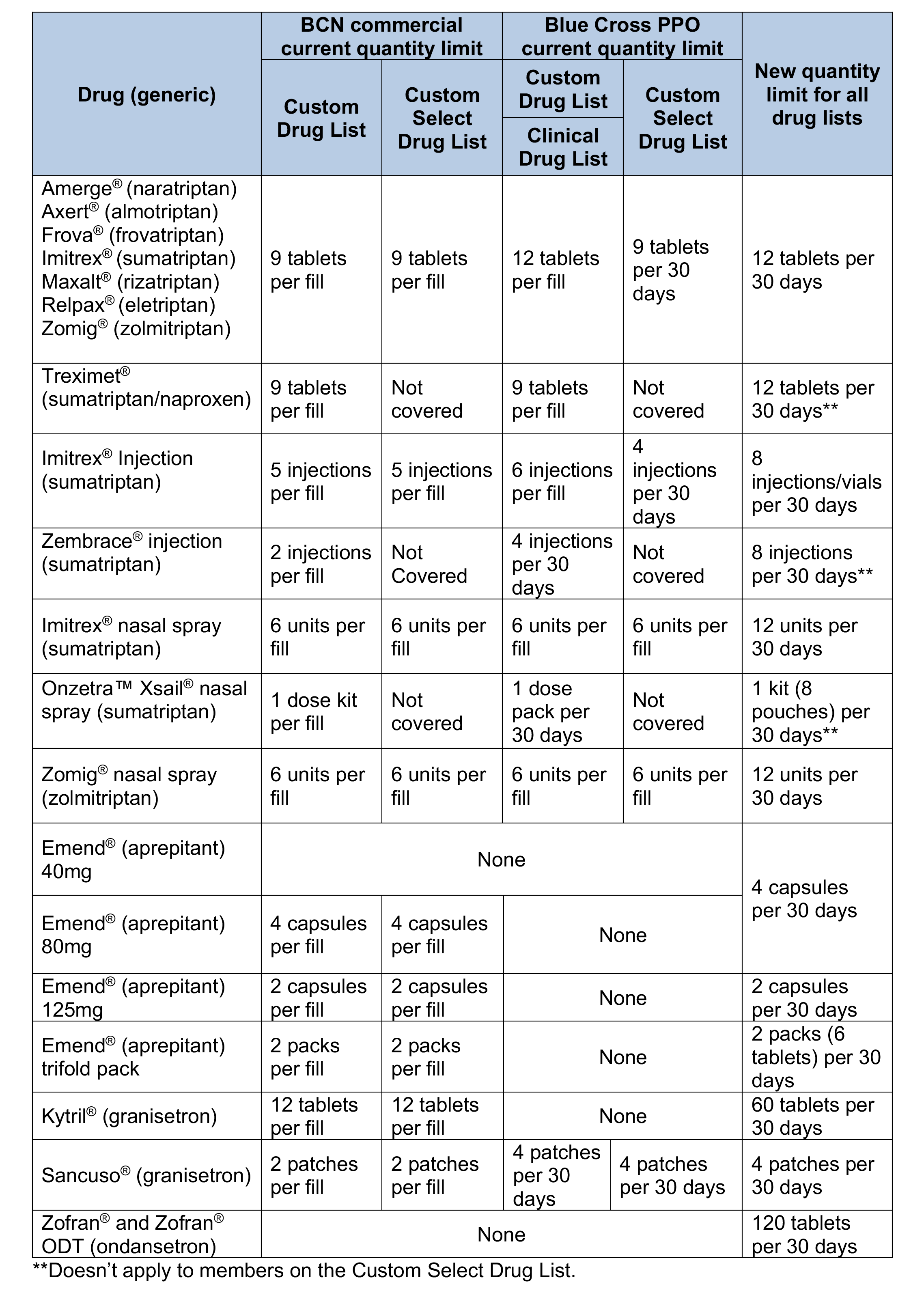
Drugs on the Clinical, Custom and Custom Select Drug Lists that will have quantity limits
These drugs will have changes to the amount that can be filled.
|







