
Forward to a friend |
Subscribe | The Record Archive | Contacts | bcbsm.com | Print this article
|
December 2023
Benefit Explainer has new payability limitation for Primary or Secondary DiagnosisOn Nov. 20, 2023, we added Primary or Secondary Diagnosis as a new payability limitation to Benefit Explainer. When users view standalone Primary or Secondary Diagnosis, Primary Diagnosis or Any Diagnosis rules, the information bubble icon they see will read Applies or Does not apply. 
When users hover over the icon, they’ll see how the different rules apply to an outpatient facility claim billed with the same HCPCS code. When the bubble reads Applies it means the following for each rule: Standalone Primary Diagnosis – The diagnosis restriction on the outpatient facility claim will only be based on the primary diagnosis code billed. Standalone Primary or Secondary Diagnosis – The diagnosis restriction on the outpatient facility claim will be based on the primary diagnosis or the second diagnosis code billed. Standalone Any Diagnosis – The diagnosis restriction on the outpatient facility claim will be based on any diagnosis code billed. When the icon reads Does not apply for any of the above standalone diagnosis limitations, a diagnosis restriction won’t be applied to the outpatient facility claim. Below is an example of what users will see. The example is for procedure code J0185 on the Medical/Payment Policy tab under Coverage Limitations, Medical, Primary Diagnosis. When a user hovers over the icon, information on the diagnosis type appears. 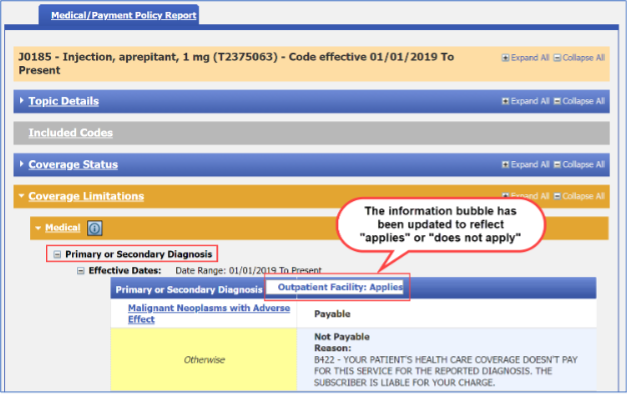
Background Facility outpatient claims are required to be billed with a HCPCS code. During claims processing, the Medical Policy Primary Diagnosis rule for the HCPCS code is applied to the outpatient facility claim. Health care providers can submit up to 25 diagnoses on a facility claim. The information in the icon defines the location of the diagnosis on the facility claim that should be read to apply the Medical Policy Diagnosis rule. Note: Screenshot examples are for illustrative purposes and may not reflect actual data. |
|
No portion of this publication may be copied without the express written permission of Blue Cross Blue Shield of Michigan, except that BCBSM participating health care providers may make copies for their personal use. In no event may any portion of this publication be copied or reprinted and used for commercial purposes by any party other than BCBSM.
|