
Forward to a friend |
Subscribe | The Record Archive | Contacts | bcbsm.com | Print this article
|
July 2021
Change Healthcare continues outreach to educate providers about appropriate use of procedure codesSelecting the CPT code that best reflects the complexity of an evaluation and management service can present a challenge for coders. Perhaps that’s why it’s not uncommon to make a mistake when selecting the appropriate E/M code. To help health care providers and their office staff determine which CPT procedure code best reflects the complexity of a visit, Blue Cross Blue Shield of Michigan contracted with Change Healthcare, an independent company, to implement its Coding Advisor program in 2019. Change Healthcare reviews E/M codes billed and other scenarios, such as modifier 25, observation care and nursing facility care, on claims submitted to Blue Cross. The program provides useful data insights to the provider community and works to maximize coding efficiency and accuracy through up-front education, rather than a traditional post-claim review process. In July, Change Healthcare will reach out by phone or letter to providers who submit claims to Blue Cross with E/M codes. Coding Advisor will compare the billing of those codes to the codes used by their peers through a physician profile. See an example of a physician profile at the end of this article. Throughout the course of this program, Coding Advisor will continue to monitor billing practices and send updated reports periodically. The company may contact your practice to discuss coding variances and to offer one-on-one coding education. All correspondence will be sent to you from Change Healthcare. If you have any questions, call Change Healthcare Customer Support at 1‑844‑592‑7009, Option 3. 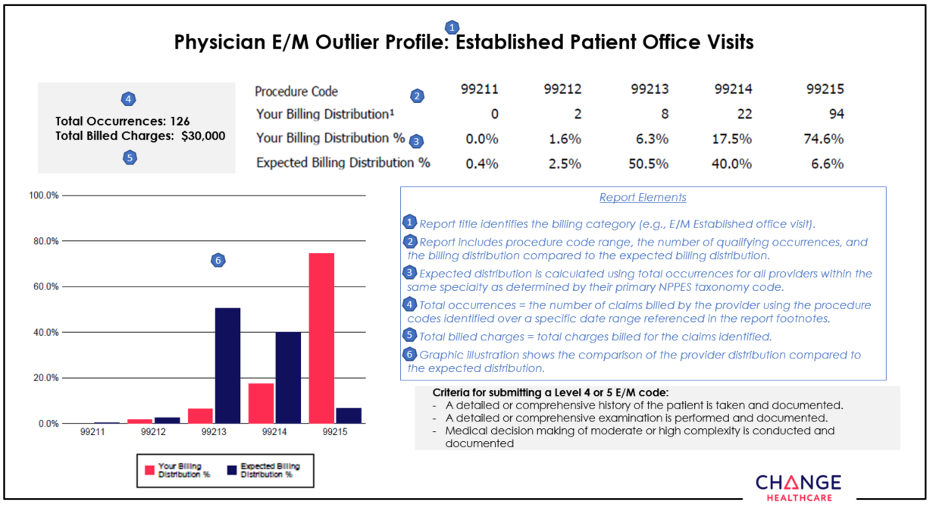
|
|
No portion of this publication may be copied without the express written permission of Blue Cross Blue Shield of Michigan, except that BCBSM participating health care providers may make copies for their personal use. In no event may any portion of this publication be copied or reprinted and used for commercial purposes by any party other than BCBSM.
|